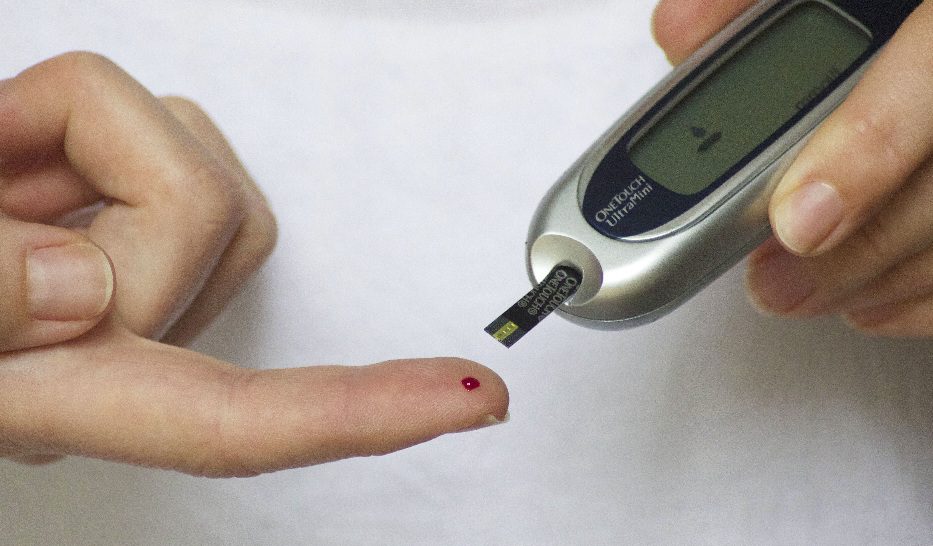
Image by Tesa Robbins from Pixabay
For years, a diagnosis of Type 2 diabetes was seen as a lifelong sentence of progressive medication. However, as we move through 2026, the narrative has fundamentally changed. The UK Diabetes Prevention 2026 strategy is no longer just about “halt and hold”; it is about remission. With the expansion of the NHS “soups and shakes” diet and revolutionary new prescribing guidelines, thousands of Britons are now successfully pushing their diabetes into reverse.
The Shift in UK Diabetes Prevention 2026
In 2026, Diabetes UK and the NHS have solidified the definition of remission: achieving an HbA1c level of less than 48mmol/mol without the need for diabetes medication for at least three months. This isn’t just a clinical goal; it’s a lifestyle revolution that is becoming the gold standard for newly diagnosed patients.
The UK Diabetes Prevention 2026 initiative has also seen a massive rollout of the Healthier You: NHS Diabetes Prevention Programme. This program now identifies “at-risk” individuals earlier than ever, using digital tools to provide personalized coaching on nutrition and physical activity before the condition even develops.
A Landmark Update in NICE Guidelines
A major pillar of the 2026 strategy is the updated NICE NG28 guideline. In a significant shift, SGLT2 inhibitors are now recommended as a first-line treatment alongside metformin for many patients.
This change is crucial because Type 2 diabetes rarely travels alone. As we established in our guide on Hypertension UK 2026, high blood pressure and high blood sugar create a “perfect storm” for the heart. The 2026 NICE update acknowledges this by prioritizing medications that offer cardiovascular and renal (kidney) protection, ensuring that managing your sugar also protects your heart.
The Role of SGLT2 Inhibitors: A 2026 Breakthrough
One of the most significant technical updates in UK Diabetes Prevention 2026 is the widespread adoption of SGLT2 inhibitors (such as Dapagliflozin). Previously reserved for advanced cases, these are now being used much earlier in the “Path to Remission.”
What makes this a 2026 game-changer is how the drug works. Unlike older medications that force the body to produce more insulin, SGLT2 inhibitors encourage the kidneys to filter excess sugar out of the blood and into the urine. This process not only lowers blood glucose levels but also aids in modest weight loss and significantly reduces blood pressure.
This “triple benefit” is why the latest UK Diabetes Prevention 2026 guidelines prioritize these drugs for patients who also struggle with the issues we highlighted in our guide on UK Cholesterol Guidelines 2026. By protecting the kidneys and heart simultaneously, clinicians are now treating the patient as a whole system rather than just a set of blood sugar numbers. This is vital because managing blood sugar is a key factor in preventing the long-term cognitive decline we discussed in our guide on Vascular Dementia UK 2026.

Image by Couleur from Pixabay
The “Path to Remission” Program
The most talked-about development in UK Diabetes Prevention 2026 is the national expansion of the NHS Type 2 Diabetes Path to Remission Programme.
What it is: A low-calorie “Total Diet Replacement” (TDR) consisting of nutritionally complete soups and shakes for 12 weeks.
The Result: Clinical trials show that nearly half of the participants who achieved significant weight loss (around 15kg) saw their Type 2 diabetes go into remission.
Access in 2026: Originally a pilot, this program is now available across every Integrated Care Board (ICB) in England, helping thousands move away from daily tablets.
Technology: Continuous Glucose Monitoring (CGM) for All?
By 2026, Continuous Glucose Monitoring (CGM) technology has moved from a specialist tool for Type 1 patients to a standard preventative asset for many with Type 2. Devices like the FreeStyle Libre 3 provide real-time data to a smartphone, allowing users to see exactly how a high-carb meal or a brisk walk affects their sugar levels. This “biofeedback” is proving to be a game-changer for long-term behavioral change.
Actionable Prevention Steps for 2026
If you are currently at risk, your UK Diabetes Prevention 2026 toolkit should include:
The 30g Fibre Goal: Increasing fibre is the “unsung hero” of 2026 nutrition. It slows sugar absorption and improves the gut microbiome, which is vital for insulin sensitivity.
Muscle Over Metrics: While weight is important, 2026 guidelines emphasize resistance training. Building muscle mass provides a larger “sink” for glucose, helping to keep your blood sugar stable even when you aren’t exercising.
Know Your Risk Score: Don’t wait for symptoms like thirst or fatigue. Use the Know Your Risk tool to see if you are eligible for the NHS prevention programme.
Debunking 2026 Diabetes Myths: What the Science Says
As UK Diabetes Prevention 2026 trends grow, so does misinformation. In 2026, the NHS is working hard to debunk three specific myths that often prevent people from reaching remission:
Myth 1: “You must avoid all fruit.”
In 2026, the advice is about the matrix of the food. While fruit juices should be avoided due to rapid sugar spikes, whole fruits (especially berries and apples) are encouraged. The fibre in the whole fruit slows down sugar absorption, making it a safe and essential part of a preventative diet.
Myth 2: “Diabetes is purely genetic.”
While genetics play a role, the UK Diabetes Prevention 2026 data shows that lifestyle factors, specifically visceral fat (fat around the organs) are the primary triggers. The “Path to Remission” program proves that by losing just 10-15% of your body weight, many can “switch off” the genetic predisposition.
Myth 3: “Remission means you are cured.”
It is vital to understand that “remission” is not a “cure.” If a patient returns to high-sugar, low-activity habits, the diabetes will return. The 2026 strategy emphasizes that remission is a “state of management” that requires ongoing healthy habits to maintain.
Image by oswaldoruiz from Pixabay
Conclusion
The story of UK Diabetes Prevention 2026 is one of hope and empowerment. By leveraging the latest NICE guidelines, the NHS Path to Remission, and real-time monitoring technology, you can take control of your metabolic health. Remember, your heart, your brain, and your blood sugar are all connected. Managing one is the first step to protecting them all.
Sources:
NICE: Type 2 diabetes in adults: management (NG28 2026 Update)
NHS Healthier You: NHS Diabetes Prevention Programme Success
Diabetes UK: Understanding Diabetes Remission in 2026
Healthcare Management UK: Major Changes to Type 2 Diabetes Treatment
